Table of Contents
Introduction
“Are ear infections contagious?” This question is frequently asked, especially during cold and flu season. While ear infections themselves are not directly contagious, the viruses and bacteria that cause them can spread easily. So, how do ear infections spread, and what can you do to protect yourself? Here are the causes of ear infections, their transmission routes, and effective prevention methods!
Are Ear Infections Contagious?
Ear infections, particularly otitis media, are not directly contagious; however, the bacteria and viruses that cause these infections can spread from person to person (Block, n.d.). Upper respiratory infections, which are commonly caused by contagious pathogens such as Streptococcus pneumoniae or Haemophilus influenzae, often precede ear infections, leading to inflammation and fluid buildup in the middle ear (Musher, 2003). Research indicates that while ear infections themselves do not spread between individuals, the underlying infections that contribute to their development, such as colds and flu, are highly transmissible (Shaw, 2024).
Studies also highlight that bacterial colonization in the nasal passages can increase the risk of developing ear infections in close contacts, particularly among children in daycare settings (Fisher, 1929). Additionally, while fungal and mold-related ear infections (otomycosis) are not contagious, they can thrive in shared moist environments (Vennewald & Wollina, 2005). Nanotechnology-based treatments are being explored to improve the management of chronic and recurrent ear infections (Gheorghe et al., 2021).
Overall, while ear infections themselves do not spread, the contagious pathogens that lead to them can be transmitted, increasing the likelihood of secondary infections in susceptible individuals.
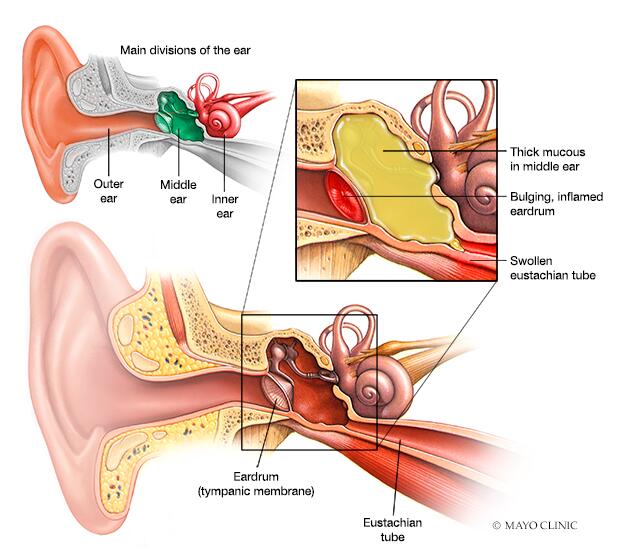
Causes of Ear Infections
Ear infections, medically known as otitis, are caused by a variety of factors, including bacterial and viral pathogens, anatomical predispositions, and environmental influences. These infections can affect different parts of the ear, including the outer ear (otitis externa), middle ear (otitis media), and inner ear (otitis interna).
1. Bacterial and Viral Infections
One of the primary causes of ear infections is bacterial or viral infections, which often originate in the upper respiratory tract. The most common bacterial culprits include Streptococcus pneumoniae and Haemophilus influenzae (Musher, 2003). Viral infections such as the flu and common cold can lead to inflammation in the Eustachian tubes, trapping fluid and creating an environment conducive to bacterial growth (Fisher, 1929).
Read: Supraglenoid Tubercle & Biceps Brachii: Anatomy and Function
2. Eustachian Tube Dysfunction
The Eustachian tubes, which connect the middle ear to the throat, play a crucial role in regulating air pressure and draining fluids. When these tubes become blocked due to allergies, sinus infections, or swelling from colds, fluid accumulates in the middle ear, increasing the risk of infection (Block, n.d.). Infants and young children are particularly susceptible due to their shorter and more horizontal Eustachian tubes (Shaw, 2024).
3. Environmental and Lifestyle Factors
Several external factors contribute to ear infections, including:
- Exposure to secondhand smoke – Inhalation of cigarette smoke can cause irritation and inflammation of the respiratory tract, leading to increased susceptibility to ear infections (Vennewald & Wollina, 2005).
- Frequent pacifier use – Studies suggest that prolonged pacifier use increases the risk of middle ear infections by altering pressure in the Eustachian tubes (Gheorghe et al., 2021).
- Swimming in contaminated water – Known as swimmer’s ear (otitis externa), this type of infection occurs when bacteria or fungi from water enter the ear canal (Shaw, 2024).
4. Allergies and Sinus Infections
Allergic reactions to pollen, dust, and pet dander can cause nasal congestion and swelling of the Eustachian tubes, leading to fluid buildup and infection (Block, n.d.). Similarly, chronic sinus infections increase the likelihood of bacterial migration to the ear, exacerbating the risk of middle ear infections (Musher, 2003).
Table 1: Causes of Ear Infections and Their Effects
| Cause | Mechanism | Risk Factors |
|---|---|---|
| Bacterial infections | Bacteria enter the middle ear, causing inflammation | Upper respiratory infections, weak immunity |
| Viral infections | Viral-induced swelling blocks Eustachian tubes | Cold, flu, RSV virus |
| Eustachian tube dysfunction | Fluid accumulation creates a breeding ground for bacteria | Young children, sinus infections |
| Environmental exposure | Smoke, allergens, and pacifier use increase risk | Secondhand smoke, allergies, daycare |
| Water exposure | Trapped moisture promotes bacterial/fungal growth | Swimming, poor ear hygiene |
How Do Ear Infections Spread?
Ear infections themselves are not directly contagious, but the bacteria and viruses that cause them can spread from person to person. Most ear infections occur as secondary infections following upper respiratory illnesses, which are highly transmissible. These infections primarily spread through airborne droplets, direct contact, and environmental factors that facilitate bacterial or viral colonization in the nasal passages and throat (Block, n.d.; Musher, 2003).
1. Transmission of Viral and Bacterial Pathogens
The primary mode of spread for ear infections is through the transmission of respiratory pathogens, which can lead to inflammation and fluid buildup in the middle ear. Common bacteria like Streptococcus pneumoniae and Haemophilus influenzae can colonize the nose and throat, eventually traveling to the Eustachian tubes and causing an infection (Fisher, 1929). Similarly, viral infections like influenza and respiratory syncytial virus (RSV) can inflame the airways and contribute to the blockage of the Eustachian tubes, leading to secondary bacterial infections (Shaw, 2024).
Read: What is Triple-Negative Breast Cancer (TNBC)
2. Airborne and Direct Contact Spread
Ear infections are often preceded by colds or flu, which spread through:
- Airborne droplets: When an infected person coughs or sneezes, respiratory droplets containing viruses and bacteria can be inhaled by others.
- Direct contact: Touching contaminated surfaces (e.g., doorknobs, shared toys) and then touching the nose or mouth can facilitate the spread of pathogens that contribute to ear infections (Vennewald & Wollina, 2005).
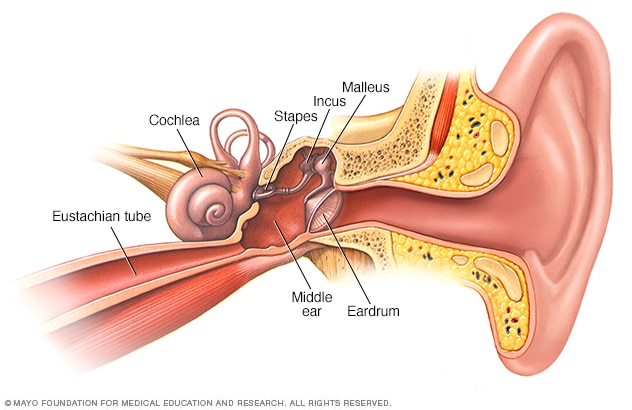
3. Environmental and Lifestyle Factors
Several environmental and lifestyle factors increase the likelihood of pathogen transmission and ear infections:
- Daycare settings and crowded environments: Children in daycare are more exposed to respiratory infections, making them more prone to developing ear infections (Gheorghe et al., 2021).
- Poor hand hygiene: Lack of proper handwashing increases the risk of transferring bacteria and viruses that can lead to respiratory and ear infections.
- Exposure to secondhand smoke: Smoke irritates the nasal passages and can cause inflammation, making it easier for infections to develop (Musher, 2003).
4. Secondary Spread Through Sinus and Nasal Infections
Sinus and nasal infections can indirectly contribute to ear infections. Congestion and inflammation can cause mucus buildup, blocking the Eustachian tubes and trapping bacteria inside the middle ear, leading to infection (Block, n.d.).
Table 2: Transmission Methods of Ear Infections
| Transmission Mode | Mechanism | Examples |
|---|---|---|
| Airborne droplets | Inhalation of virus/bacteria after a cough/sneeze | Flu, RSV, cold viruses |
| Direct contact | Touching contaminated surfaces and transferring pathogens | Shared toys, doorknobs, personal contact |
| Environmental exposure | Polluted air or smoke weakens immunity | Secondhand smoke, allergens |
| Daycare and schools | Close contact increases pathogen exposure | High infection rates among children |
| Sinus and nasal infections | Blocked Eustachian tubes trap bacteria | Chronic sinusitis, allergies |
Symptoms and Risk Factors of Ear Infections
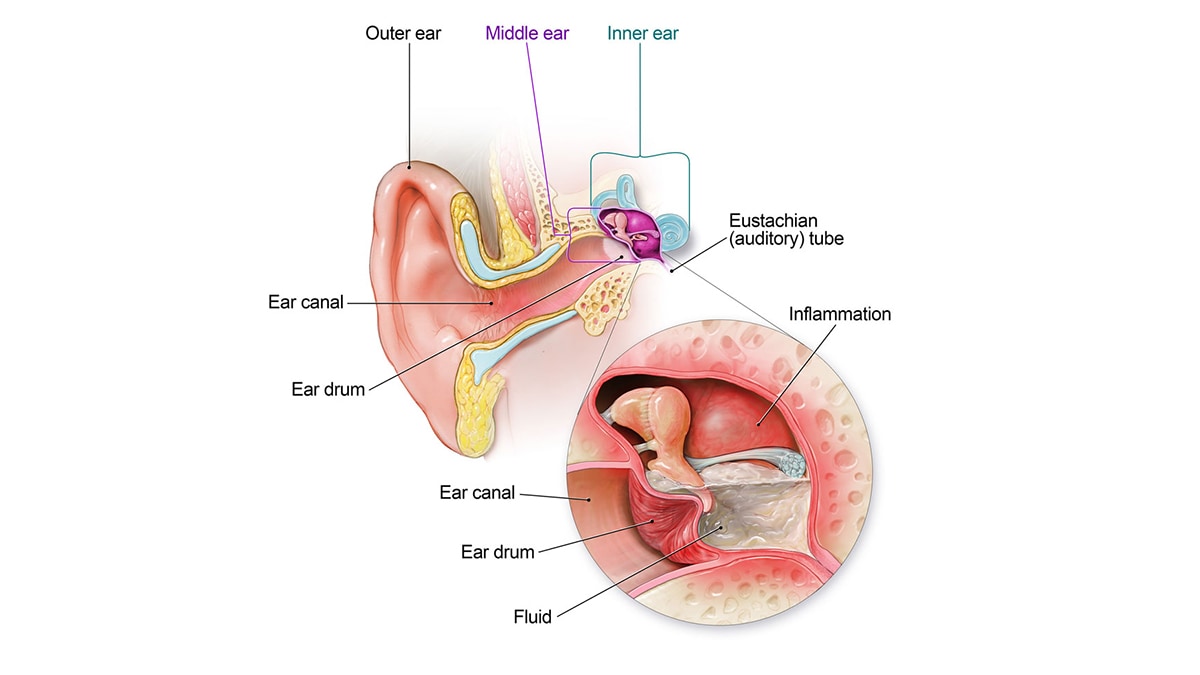
Ear infections, or otitis, present with a range of symptoms depending on the affected part of the ear—outer (otitis externa), middle (otitis media), or inner ear (otitis interna). These infections can be caused by bacterial, viral, or fungal pathogens and are influenced by various risk factors, including age, environmental conditions, and underlying health conditions (Block, n.d.; Musher, 2003).
1. Common Symptoms of Ear Infections
a) Symptoms of Middle Ear Infection (Otitis Media)
- Ear pain (otalgia), which worsens when lying down
- Fluid drainage from the ear (otorrhea)
- Hearing difficulties due to fluid buildup
- Fever, usually in bacterial infections
- Irritability and difficulty sleeping (common in children)
- Loss of balance in severe cases (Shaw, 2024)
b) Symptoms of Outer Ear Infection (Otitis Externa or Swimmer’s Ear)
- Pain when touching or pulling the ear
- Itching in the ear canal
- Swelling and redness around the ear
- Fluid or pus discharge
- Partial hearing loss due to swelling (Vennewald & Wollina, 2005)
Read: Food Poisoning vs Stomach Bug: Understanding the Differences
c) Symptoms of Inner Ear Infection (Otitis Interna or Labyrinthitis)
- Severe dizziness (vertigo)
- Nausea and vomiting
- Tinnitus (ringing in the ear)
- Hearing loss in one or both ears
- Difficulty maintaining balance (Gheorghe et al., 2021)
2. Risk Factors for Ear Infections
Several factors increase the likelihood of developing ear infections. These risk factors include anatomical differences, immune system health, and environmental exposures.
a) Age and Anatomy
Young children are more susceptible to ear infections because their Eustachian tubes are shorter and more horizontal, making it easier for fluid and bacteria to accumulate (Fisher, 1929).
b) Environmental and Lifestyle Factors
- Daycare and school environments – Close contact with other children increases exposure to respiratory infections.
- Secondhand smoke exposure – Smoke irritates the respiratory tract, increasing the risk of infections.
- Frequent pacifier use – Linked to higher rates of middle ear infections in infants (Musher, 2003).
c) Medical Conditions and Allergies
- Chronic sinus infections – Nasal congestion can block the Eustachian tubes.
- Weakened immune system – Individuals with compromised immunity are more prone to infections.
- Seasonal allergies – Cause inflammation that affects ear drainage (Block, n.d.).
Table 3: Symptoms and Risk Factors of Ear Infections
| Category | Symptoms | Risk Factors |
|---|---|---|
| Middle Ear Infection | Ear pain, fever, fluid drainage | Young children, pacifier use, daycare |
| Outer Ear Infection | Itching, pain when touched, swelling | Swimming, moisture exposure, ear picking |
| Inner Ear Infection | Vertigo, nausea, tinnitus, hearing loss | Viral infections, weakened immunity |
| General Risk Factors | N/A | Smoke exposure, allergies, chronic sinusitis |
Prevention Methods and Treatment Options for Ear Infections
Ear infections are a common health concern, particularly among young children, and can result from bacterial, viral, or fungal infections. Prevention focuses on reducing risk factors, while treatment varies depending on the type and severity of the infection. Proper management is essential to prevent complications such as chronic infections or hearing loss (Block, n.d.; Musher, 2003).
1. Prevention Methods
a) Vaccinations
- Pneumococcal and influenza vaccines reduce the risk of bacterial and viral infections that can lead to ear infections (Shaw, 2024).
- Haemophilus influenzae type b (Hib) vaccine helps protect against a leading cause of bacterial ear infections (Musher, 2003).
b) Hygiene and Lifestyle Changes
- Frequent handwashing to prevent the spread of cold and flu viruses.
- Avoiding secondhand smoke since exposure can irritate the nasal passages and increase the likelihood of infections (Vennewald & Wollina, 2005).
- Reducing pacifier use in infants, as it has been linked to an increased risk of ear infections (Gheorghe et al., 2021).
c) Managing Allergies and Sinus Issues
- Controlling allergies with antihistamines or avoiding triggers to reduce nasal inflammation.
- Treating sinus infections promptly to prevent bacterial migration to the middle ear (Block, n.d.).
2. Treatment Options
a) Medications
- Antibiotics (e.g., amoxicillin) are prescribed for bacterial infections but are not effective for viral causes (Musher, 2003).
- Pain relievers like ibuprofen or acetaminophen help manage discomfort and fever (Shaw, 2024).
- Antifungal treatments are used for otomycosis (fungal ear infections) (Vennewald & Wollina, 2005).
b) Ear Tubes (Tympanostomy Tubes)
- In cases of recurrent infections, small tubes may be surgically placed in the eardrum to aid fluid drainage and prevent infections (Gheorghe et al., 2021).
c) Home Remedies and Supportive Care
- Warm compresses can relieve pain and reduce inflammation.
- Keeping the ear dry helps prevent swimmer’s ear (otitis externa).
- Rest and hydration support the immune system in fighting infections (Block, n.d.).
Table 4: Prevention and Treatment Approaches
| Approach | Methods | Effectiveness |
|---|---|---|
| Vaccinations | Pneumococcal, flu, Hib vaccines | High—prevents many infections |
| Hygiene Practices | Handwashing, smoke avoidance | Moderate—reduces risk |
| Medical Treatments | Antibiotics (bacterial), antifungals | Effective if pathogen identified |
| Surgical Intervention | Tympanostomy tubes for chronic infections | High for recurrent infections |
| Home Remedies | Warm compress, hydration, ear drying | Supportive—relieves symptoms |
Frequently Asked Questions (FAQ) About Ear Infections
1. What are the most common causes of ear infections?
Ear infections are primarily caused by bacterial or viral pathogens that originate in the upper respiratory tract. Common bacteria include Streptococcus pneumoniae and Haemophilus influenzae, while viral infections such as the flu or RSV can trigger inflammation in the Eustachian tubes, leading to fluid buildup in the middle ear (Musher, 2003; Shaw, 2024). Other risk factors include sinus infections, allergies, secondhand smoke exposure, and swimming in contaminated water (Block, n.d.).
2. Are ear infections contagious?
The infection itself is not directly contagious, but the bacteria and viruses that lead to it can spread from person to person. For example, a cold or flu virus can be transmitted through respiratory droplets, and if it causes inflammation in the nasal passages and Eustachian tubes, it may lead to an ear infection (Vennewald & Wollina, 2005). Practicing good hygiene, such as washing hands frequently and avoiding close contact with sick individuals, can help prevent ear infections (Fisher, 1929).
3. How can I tell if my child has an ear infection?
Children with ear infections often show the following symptoms:
- Ear pain, especially when lying down
- Tugging or pulling at the ear
- Fluid draining from the ear
- Fever (often with bacterial infections)
- Trouble hearing or responding to sounds
- Irritability and difficulty sleeping (Shaw, 2024; Gheorghe et al., 2021)
If symptoms persist for more than 48 hours, it is advisable to seek medical attention.
Read: Sustentaculum Tali 101: A Detailed Review
4. What are the best treatment options for ear infections?
Treatment depends on whether the infection is bacterial, viral, or fungal:
- Bacterial infections: Often treated with antibiotics such as amoxicillin.
- Viral infections: Usually self-limiting and require supportive care (e.g., pain relievers, hydration).
- Fungal infections: Require antifungal ear drops (Vennewald & Wollina, 2005).
For chronic ear infections, a doctor may recommend tympanostomy tubes to drain fluid and prevent recurrent infections (Gheorghe et al., 2021).
5. How can ear infections be prevented?
- Vaccinations: Pneumococcal, influenza, and Hib vaccines can reduce infection risks.
- Good hygiene: Regular handwashing and avoiding close contact with sick individuals.
- Breastfeeding: Provides immunity-boosting antibodies for infants.
- Avoiding smoke exposure: Reduces respiratory irritation.
- Managing allergies: Prevents nasal congestion and Eustachian tube blockage (Block, n.d.; Musher, 2003).
Conclusion: Understanding and Managing Ear Infections
Ear infections are a prevalent health issue, particularly among young children, and can arise from bacterial, viral, or fungal pathogens. While the infections themselves are not directly contagious, the viruses and bacteria that cause them can spread through respiratory droplets, direct contact, and environmental factors (Musher, 2003; Shaw, 2024).
Causes of ear infections often include upper respiratory infections, Eustachian tube dysfunction, allergies, and environmental exposures such as secondhand smoke and frequent swimming (Fisher, 1929; Block, n.d.). The symptoms vary based on the affected part of the ear but commonly include ear pain, fever, fluid discharge, and hearing difficulties. Inner ear infections may also lead to dizziness and balance issues (Gheorghe et al., 2021).
Risk factors include age (infants and young children are more susceptible), frequent respiratory infections, poor hygiene, and chronic sinus conditions (Vennewald & Wollina, 2005). Preventative measures such as vaccinations (pneumococcal, flu, and Hib vaccines), hand hygiene, breastfeeding, and reducing exposure to irritants can help lower infection risks.
Treatment depends on the underlying cause:
- Bacterial infections respond well to antibiotics like amoxicillin.
- Viral infections require symptom management and usually resolve on their own.
- Fungal infections are treated with antifungal ear drops (Vennewald & Wollina, 2005).
For chronic or recurrent infections, tympanostomy tubes may be recommended to aid drainage and reduce the likelihood of complications (Gheorghe et al., 2021).
Final Thoughts
Ear infections, while common, can be effectively prevented and managed through a combination of medical intervention, lifestyle modifications, and good hygiene practices. Understanding their causes, symptoms, and treatment options allows individuals and caregivers to take proactive measures to reduce their occurrence and severity. Continued research, including advancements in nanoparticle-based treatments, offers promising new approaches for more efficient and targeted ear infection therapies in the future (Gheorghe et al., 2021).
Read: What is Recumbency? Its Role in Healthcare
References
Block, S. L. (n.d.). Ear infection. Retrieved from https://www.calvarypediatrics.com/medical-conditions/e/
Fisher, J. H. (1929). Upper respiratory and middle ear infections: A bacteriologic and experimental study. The Journal of Infectious Diseases. Retrieved from https://www.jstor.org/stable/30083581
Gheorghe, D. C., Niculescu, A. G., & Bîrcă, A. C. (2021). Nanoparticles for the treatment of inner ear infections. Nanomaterials, 11(5), 1311. Retrieved from https://www.mdpi.com/2079-4991/11/5/1311
Musher, D. M. (2003). How contagious are common respiratory tract infections? New England Journal of Medicine. Retrieved from https://www.nejm.org/doi/abs/10.1056/NEJMra021771
Shaw, J. A. (2024). Contagious diseases. Springer. Retrieved from https://link.springer.com/chapter/10.1007/978-3-031-52346-5_2
Vennewald, I., & Wollina, U. (2005). Cutaneous infections due to opportunistic molds: Uncommon presentations. Clinics in Dermatology. Retrieved from https://www.sciencedirect.com/science/article/pii/S0738081X05000209



What are the best ways to prevent ear infections in young children, especially if they’re in daycare? I’m worried about how quickly infections spread there.
Totally get your worry about daycare germs! Here’s the short and sweet on preventing ear infections:
Get Vaccinated: Make sure your kid has all their shots, especially for pneumonia and flu.
Wash Hands, Wash Hands, Wash Hands: Super important for everyone, especially before eating and after sneezes.
No Smoke: Keep your child away from cigarette smoke.
Easy on Pacifiers: Try to cut back on pacifier use, especially as they get older.
Handle Allergies: If they have allergies, get them treated to keep noses clear.
These simple steps can really help keep those ear infections away!
Are ear infections contagious only because of the viruses and bacteria that cause them, or can the infection itself spread directly from person to person? Just trying to understand how careful I need to be around someone with an ear infection.
That’s a great question! Ear infections themselves, like the fluid buildup and inflammation in the ear, are not directly contagious. You can’t “catch” an ear infection from someone else in the same way you’d catch a cold.
However, you’re absolutely right to be curious about the underlying causes. The viruses and bacteria that lead to ear infections (like those causing colds, flu, or strep throat) are highly contagious. These germs spread through things like coughing, sneezing, or touching contaminated surfaces.
So, while the ear infection itself won’t jump from person to person, if you’re around someone with an ear infection, they likely have a contagious respiratory illness that could spread to you. If you catch that cold or flu, it could then potentially lead to an ear infection in you, especially if you’re susceptible (like young children often are).
Think of it this way: The ear infection is a result of a contagious germ, not the contagious thing itself. So, practicing good hygiene (like handwashing) and avoiding close contact with sick people are still the best ways to protect yourself!
This article really helped me understand that while ear infections themselves aren’t contagious, the colds and flu that lead to them can spread easily. Good to know for keeping kids safe during cold season!
I liked the breakdown of symptoms for different types of ear infections. It’s good to know when to see a doctor, especially with kids who can’t explain what’s wrong.
Helpful overview. I didn’t realize secondhand smoke could increase the risk of ear infections.
Thanks, very clear and useful info!
Thanks. Now I know what is it.